Pet Of The Year 2025
The shortlist for Pet Of The Year 2025 is here!
Take a look at our top 12 to refresh your memory and then vote for your favourite by liking their photo on our facebook post.
Voting closes at 9am on Thursday 12th February
Bella’s Battle with Evans Syndrome: How Blood Donor Dogs Helped Save Her Life—Twice!
Evans syndrome is a rare but serious autoimmune condition in which the body’s own immune system mistakenly attacks and destroys both red blood cells and platelets. The loss of red blood cells leads to anaemia, causing weakness and lethargy, while the destruction of platelets increases the risk of spontaneous bleeding. If left untreated, the condition can progress rapidly and become life-threatening.
Blood products play a vital role in the management of Evans syndrome, though they do not offer a cure. Instead, they serve as a crucial supportive measure, stabilising the patient and buying valuable time for immunosuppressive treatment, most commonly steroids, to take effect. These medications work by reducing the immune response and halting further destruction of blood cells. Once the immune system is suppressed, the bone marrow can begin to replenish the lost red blood cells and platelets.
A notable case in our practice involved Bella, a four-year-old Maltese, who was diagnosed with Evans syndrome.
In May 2024, Bella was being cared for by her owner’s mum while her owner was on holiday in Canada. Four days in, Bella’s owner received a concerned phone call from her mum, saying Bella wasn’t eating and didn’t seem quite herself. She thought it might be due to separation anxiety, as Bella had acted like this before. Unfortunately, a day later, Bella’s owner received the devastating news that Bella had collapsed and was being rushed into the veterinary hospital. After blood tests, the vets discovered that her red blood cell count (also known as the packed cell volume) was just 5%, in a healthy dog this typically ranges from 35–50%. Bella was then diagnosed with Immune-Mediated Haemolytic Anaemia (IMHA) – an autoimmune disease in which the immune system mistakenly attacks and destroys the body’s own red blood cells. It was also discovered that she has a rare blood type, so Pet Blood Bank UK were contacted and organised a donor for a blood transfusion, which ultimately saved her life… for the first time.
When her owner returned home, Bella was discharged from the veterinary hospital and transferred to our care here at Shepton Vets, where we began stabilising her condition and gradually reducing her daily medication from eight tablets a day. After blood tests every 2–4 weeks for seven months, she was medication-free and healthy.
Unfortunately, four months later, in April 2025, she became lethargic and declined so rapidly that the medication being administered couldn’t act quickly enough for her body to respond. Bella was immediately brought to us after collapsing at home. After further tests, she was diagnosed with Evans syndrome. Her red blood cell levels were dropping rapidly, so a donor dog was urgently needed for a blood transfusion. Panda, a two-year-old Lurcher belonging to a member of staff in our farm office, stepped up to be a hero by donating blood—and once again, Bella’s life was saved by the kindness of another.
Bella now visits us every four weeks for check-ups to monitor her blood and reduce her medication to a manageable dose. Her condition is currently stable, and to look at her, you wouldn’t know she is living with a chronic illness. She’s a very happy and sweet girl who still loves to cause mischief. Bella was previously a ‘Pets As Therapy’ dog and always has to say hello to everyone on her walks and visits to us.
With timely intervention, including the use of blood products and immunosuppressive therapy, Bella’s condition stabilised. In some cases, patients can be gradually weaned off steroids, while others may require long-term, low-dose therapy to prevent relapse.
The use of blood products, whether for autoimmune conditions like Evans syndrome or toxicities such as rodenticide ingestion, highlights the importance of prompt diagnosis and tailored treatment in veterinary emergency care. It also demonstrates the vital role of organisations like Pet Blood Bank UK, who provide life-saving supplies in critical moments.
Pet Blood Bank UK exists to help save the lives of pets in need by providing a blood service for vets. They operate 24 hours a day, seven days a week, to ensure blood is always available. Donation sessions are hosted at various locations across the country, where pet owners can bring their dogs to donate blood in a calm and stress-free environment. One of these locations is our Wells branch, where we host sessions every eight weeks – the next one being Saturday 19th July.
To find out more, check eligibility, and sign your dog up, visit the Pet Blood Bank
website: www.petbloodbankuk.org
Blood transfusions help to save the lives of thousands of dogs like Bella every year. Every unit of blood can help save the lives of up to four other dogs. Sign your dog up to be a lifesaver today.

A New View on Life: Boris the One-Eyed Farm Cat’s Miraculous Recovery
Boris is a farm cat, but no ordinary farm cat. Firstly, he’s a much adored, affectionate member of his owners’ family, and secondly, he has staged a remarkable recovery from a near fatal mystery incident that led to him losing an eye and being fed through a tube for a week.
Boris’ owners inherited the 5-year-old black moggy with the beef farm that they had taken on a year ago, but he quickly became a much-loved member of the team. So, his owners wanted to do all they could when he was found almost lifeless in a sorry state one morning. He was rushed to the vets for an emergency appointment, almost unrecognisable from the handsome tom he was known to be, due to significant wounds and damage to his head.
Because of the extent of his injuries, swelling and bleeding, it was initially thought that Boris had collided head on with a car. Boris was bleeding from several wounds around his mouth and his head had swollen up resembling a football, whilst his eyes were very bloody and damaged. The first priority was to stabilise him and get him as comfortable as possible with strong pain relief. Then, step by step, the severity of his damage needed to be assessed very carefully, with X-rays and a gentle hands-on examination.
It seemed as though Boris couldn’t see and he could barely breathe due to the swelling around his nose. There was no suggestion of significant damage or fractures elsewhere on his body, but it was too dangerous and high risk to anaesthetise him in order to check his jaw and skull fully in the first 48 hours. Instead, he was hospitalised continuing pain killers, alongside antibiotics, and was intensively assessed for any deterioration.
Two days on from the initial trauma, some of the swelling around his eyes had improved, but he showed no interest in eating and due to the damage around his mouth it wasn’t clear whether it was physically possible for him to. With great care, Boris was anaesthetised successfully allowing the veterinary team to assess his head thoroughly. Surprisingly, an X-ray showed no jaw or skull fractures but there were several wounds around his mouth that needed to be cleaned up. It seemed like both of his eyes were not working correctly and that his right eye was so badly damaged it would need to be removed at a later stage. His claws were not scuffed which did not suggest a car accident, and he had several puncture wounds around his chin that were reminiscent of an animal attack.
Whilst under the anaesthetic and after being cleaned up, it was decided to place a feeding tube for Boris so he could receive nutrition. The swelling around his mouth was still so great that he would probably not feel comfortable to eat for a while yet. A tube was surgically inserted into his oesophagus – the food tube that leads from the mouth to the stomach – and stitched and dressed in place around his neck.
Over the next few days, the swelling around his head receded impressively, he could receive medication as well as food into this tube and this was helping to build up his strength. Once Boris was stable and his owners were happy and confident enough, he was allowed home to be fed through his tube following instruction from the hospital nurse. Boris’ owners took to this task brilliantly, and after a week at home he returned to the practice, much improved, for a check-up. To everyone’s delight he had started eating well and his feeding tube could be removed by the consulting nurse. However, he was still blind and it was evident that his right eye was damaged beyond repair, meaning it would need to be surgically removed.
Boris would need to adapt to be an indoor cat but his owners felt this could be possible, and everyone at the practice agreed as he was no ordinary farm cat – being happy to be kennelled in the cattery for his long period of hospitalisation and showing remarkable affection and acceptance of fuss throughout the traumatic process. The next week, Boris’ eye operation took place and the surgery was a success. He had some post surgical swelling that again transformed his face, but nothing like his initial injuries. After his final surgery and visit to the practice, Boris could put the whole ordeal behind him. It was a mystery how he had got into such a mess, but he was now fully on the mend as a happy, indoor farm cat.
Dave the Determined Chihuahua x Pomeranian
We can all feel a bit over-indulged at Christmas and maybe realise we need to stop eating quite so much. However, when 7-year-old Dave, the Chihuahua x Pomeranian, stopped eating for 3 days his owners knew something wasn’t right.
Dave is a character – loving, but also strong willed when he needs to be! And sometimes going a couple of days without eating is just how he rolls. So, when he didn’t eat for a day or two around Christmas his owners didn’t immediately question it. But when he got to day three with no appetite, they knew something was amiss, especially so when he also started vomiting. At this point Dave was booked in for a Boxing Day appointment at our Poorly Pet Clinic.
When he was seen at his appointment Dave seemed fairly bright but a little quiet compared to his usual demeanour. Other than this, the only abnormality we could find on our examination was that his eyes and gums appeared a bit yellow (jaundice), and it was this finding that meant further investigation was required. After a short discussion with his anxious owners, Dave was admitted for further tests.
There can be several reasons for a patient to be jaundiced and so vet Polly started by running some blood tests. Dave’s blood sample was processed immediately and gave us some crucial findings. They confirmed that Dave was not anaemic and had no sign of red blood cell breakdown. This helped to rule out one of the major causes of jaundice immediately. But Dave’s results did show that his liver markers were elevated so Polly was quickly able to identify that the root of Dave’s problem was likely to be related to his liver.
Dave was started in intravenous fluids, given some anti-sickness medication and then Polly performed an ultrasound examination of his liver. This immediately flagged a very unusual appearance to his gall bladder (the sack within the liver that stores bile) and further narrowed down on the cause of his ailment. Dave’s owners were informed and as he benefitted from his fluids and other medications, it was elected that he would stay in for nursing and a further work up the following day.
Dave maybe wasn’t his headstrong self the next day, but he was a little brighter for having had fluids and care overnight. The day’s mission was to establish what was going on in his gall bladder, and what plan we would have for treatment. And with this Dave underwent more imaging.
Once again, his gall bladder looked very unusual but thankfully everything else appeared fine. At this stage, we suspected that the unusual appearance of Dave’s gall bladder was most likely due to one of two possible causes. He could have a biliary mucocele, a nasty condition whether the bile becomes very thick and obstructs flow from the gall bladder. This is a condition that we can potentially manage with surgery and can often be readily diagnosed on ultrasound as it can have a very classic appearance. However, Dave’s ultrasound was not typical of a mucocele, and we felt it was also possible that he had a tumour of his gall bladder instead, which would be very difficult to treat. With two potential, quite nasty diagnoses, and no way to easily distinguish them by appearance, we needed more information. So, some samples were taken from his gall bladder by needle. These were sent to the lab, and then we waited.
The results returned. The good news was that tumour cells weren’t found. The not so-good-news was that the result wasn’t definitive. Dave was now eating very small amounts but losing weight. We spoke to his owners and discussed next options. What was elected was to progress to an exploratory abdominal surgery to investigate what was happening.
We prepped Dave for surgery and proceeded to his exploratory laparotomy. The findings were immediately interesting, and in a good way for Dave. He did indeed have a gall bladder mucocele and it had obviously ruptured, something that worsens the prognosis. However, it had turned out that fat within his abdomen had blocked the rupture and fused to it. The result was that what could have been a catastrophic infection that would have leaked into his entire abdomen was in fact confined to one focal area. His body was doing it’s very best to keep him alive!
The next stage was to resect his diseased and burst gall bladder, resect the infected fat that had saved him, and then to flush his abdomen with copious amounts of sterile saline to remove any remnants of retained infection. He was then sutured closed and finally a feeding tube was placed into his oesophagus to allow us to feed him over the following days.
The nursing team had done an incredible job to manage Dave’s blood pressure during and after his procedure and thanks to this he recovered calmly in the hospital and started tube feeds 12 hours after the conclusion of his procedure. His recovery had commenced.
Dave was hospitalised for 3 days with multiple medications and tube feeds being given regularly. Day by day he improved and when he went home, he then had follow up appointments in the practice every few days. On each occasion he weighed a bit more and looked a bit less yellow. Everything was heading in the right direction.
After 10 days Dave’s feeding tube was removed, and life was back to normal. The half a kilo that he’d originally lost had successfully been regained and Dave could breath a sigh of relief. He’d had a lucky escape, helped by his owners’ care and his body’s determination to do everything it could to keep him alive.

Remarkable Milo: A Tail of Curiosity, Courage, and Healing
*WARNING*
Graphic images at the bottom of this article.
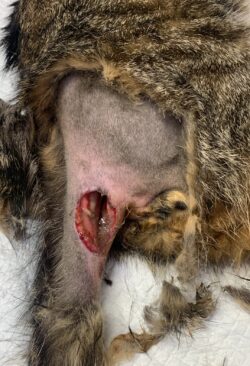
Milo is a young and curious cat who, like many cats, has lots of adventures outside of his home and who knows what they all get up to! But a few months ago, Milo came home with a painful tail, he was very sad and didn’t want to interact with his owners like he normally would, which prompted a visit to our Sunday morning clinic in Shepton. He was checked over but aside from a painful tail, nothing more was found, so he was prescribed some pain relief to make him more comfortable and was under close observation at home by his owners. When his signs hadn’t improved much, he was brought back for a recheck, this time he was even more unhappy about his tail being touched and was also experiencing some severe diarrhoea. Milo was admitted into the vets for an examination under anaesthesia and some xrays of his pelvis and tail.
Once Milo was asleep, we were able to assess him much more thoroughly. Even under anaesthetic his rectal temperature was very high, above 40 degrees Celsius and we discovered a large wound along the right side of his tail that was initially completely covered by his coat. We cleaned him up, removing the hair and other bits of debris to reveal a really deep wound around the base of his tail, that exposed the internal structures of his tail, pelvis and rectum. Sadly for Milo, the damage extended further with rupture of the rectal wall meaning the wound was further contaminated by faeces too. The only saving grace was that none of the bones appeared to be broken on the xrays.
Our team of vets and nurses can manage a significant majority of cases, but we must be aware of our limitations and identify cases that require more specialist input. We work collaboratively with specialist veterinary referral hospital when necessary and once the specialist work is done, the patients return to our care so that we can continue to support our patients and clients. The damage to Milo’s rectal wall was really serious and required urgent treatment. Without our super surgeon Martin to help us due to annual leave, the best option for Milo was to travel to a nearby referral hospital for specialist surgical repair and post-operative care.
Rectal surgery is very challenging and not without potential complications including a high risk of the surgical site breaking down, this is due to the fragile nature of the tissue, the forces that go through the fragile tissue when going to the toilet and the naturally high bacterial content of this area of the body. Unsurprisingly Milo’s rectal wound did break down a few days after surgery, which left us with very few options, other than to keep the area clean and hope that it would heal on its own. So, Milo was transferred back to our care and visited us twice a week for a sedation to clean up and flush the wound, whilst we waited to see if his own body could repair itself sufficiently. Remarkably, within three weeks the hole in the skin had closed over and within four weeks Milo was off all medication without any issues going to the toilet. A cat’s ability to heal, especially a young cat, will never fail to amaze me, within weeks, Milo’s tail looked like nothing had ever happened.




Crikey, That’s A Poorly Dog!
Poodle crossbreeds make up a large proportion of the dogs that are registered with the practice due to their desirable coat and friendly temperament. The crossbreeds we see are commonly Cockapoos, Cavapoos or labradoodles – but occasionally there are lesser known crosses encountered such as the schnoodle. The schnoodle is born when the poodle is crossed with the schnauzer, which is a characterful and charming dog in its own right. But schnauzers can be predisposed to liver and gall bladder disease, and that is exactly what the delightfully named Crikey the schnoodle had been suffering from.
Last year, blood tests picked up that Crikey had abnormally high ‘liver enzymes’ within his bloodstream. At that time, he was quite happy in himself, but earlier this summer Crikey began to become unwell. He had started to suffer from bloody diarrhoea with vomiting for a few days – known as ‘haemorrhagic gastroenteritis’. This put him completely off his food. He seemed quite sad when he arrived for his appointment at the practice—far from his usual bouncy self that everyone had come to know during his regular routine vet visits.
As everyone was quite concerned about Crikey’s demeanour, he was admitted to be hospitalised for supportive treatment that consisted of probiotic paste, anti-sickness injections, gastroprotectants and intravenous fluids. Blood tests were taken that showed his liver values had worsened further from last time and he was suffering from a degree of pancreatitis – inflammation of the digestive organ the pancreas. After 24 hours at the practice, Crikey felt a little better and hadn’t vomited, but still had terrible diarrhoea and wouldn’t eat a thing. It was decided that he would have to stay in for at least another night, but this then turned into a third night too when he didn’t pick up as everyone had hoped.
Being away from home can add to further worry for a pet owner who is already concerned about whether they will pull through, but Crikey’s owner was relieved to receive regular updates from the night nurse in the form of photos, and videos of Crikey getting all the care and comfort he needed. On the fourth day, after having extra medications added in such as appetite stimulants and further anti nausea treatments, Crikey had an in depth ultrasound scan of his gall bladder, which is closely related to both the liver and the pancreas. This scan revealed that there was a build up of sludgy, thickened bile clogging up around his liver. Samples were taken of Crikey’s bile via an ultrasound guided needle.
Whilst these samples were sent off to the external lab for further testing, Crikey was started on yet further medication, at the risk of becoming a barking pharmacy! This consisted of an antibiotic designed to act within the gall bladder, as well as a drug to help contract the bile duct, assisting flow of bile out from the gall bladder.
Pleasingly, Crikey started to respond better to these medications and appeared noticeably brighter. That evening, he even started eating – which Crikey’s owner was delighted to see in the latest evening phone update.
Results two days later ruled out any evidence of cancer, but showed that Crikey was suffering from an unusual but serious infection in his gall bladder. A type of bacteria known as Pseudomonas was grown in the lab from Crikey’s bile. This bacteria is notoriously difficult to treat and is more commonly found in nasty ear infections. This particular bug had probably travelled up from his gut, through the bile duct to enter the gall bladder and cause sludgy bile as well as discomfort and a lot of sickness!
Fortunately by this time, Crikey was well enough to go home as he had continued to eat and get stronger, but the results indicated he needed an extra antibiotic to get him back to full fitness. After a week’s course of tablets, Crikey was unbelievably back on top form, just two weeks on from a time where his owner thought he might not make it. He continues to thrive at home now on a specialised digestible and low fat diet to ease the pressure on his gut, pancreas, liver and gall bladder. Crikey, he’s a lucky dog!

Sox the Cat: From Cystitis to Surgery – A Tale of Nine Lives and Dedication
Sox the cat is not your average moggy. At six years old, this handsome black-and-white neutered tom has already faced more health challenges than most felines will in a lifetime. His journey has been one of ups and downs, late-night dashes to the vet, and a final big decision that may just have saved his life.
For the first three years of his life, Sox was the picture of health, but around his third birthday things began to change. He started to develop cystitis, an inflammation of the bladder. While humans might associate bladder problems with infection, in cats the story is usually more complicated with feline cystitis often linked to stress, with the bladder becoming inflamed even when no bacteria are present.
Sox’s bouts of cystitis came and went, leaving his owner both worried and determined to get to the bottom of things. Tests were run – urine samples, blood work and ultimately X-rays and ultrasound of his bladder – all of which came back normal. That ruled out infections and other obvious causes. So, Sox’s owner turned to the practice’s feline behaviour nurse, and together they worked on strategies to lower Sox’s stress and encourage him to drink more water.
Changes were made at home: multiple litter trays, extra water bowls dotted around the house, cosy spaces just for Sox, and even special pheromone diffusers designed to help cats feel calmer. These adjustments made a difference, and for a time, life carried on as normal.
But earlier this year, Sox faced a crisis. One morning, he simply couldn’t pass urine. In veterinary terms, he was “blocked” – his urethra obstructed, meaning no urine could leave his body. For cats, this is not only excruciatingly painful, but also rapidly life-threatening. Waste products build up in the bloodstream, and ultimately the obstruction can start to cause organ failure.
His owner rushed him to the practice where emergency treatment began. Under anaesthetic, a catheter was passed into Sox’s bladder to relieve the obstruction. He spent several days in hospital before the catheter was removed, and while his recovery was slow at first, he eventually bounced back to his cheeky self.
Life began to settle again. Sox was playing, eating, and enjoying his home comforts. But then came another blow. One day, Sox didn’t come home. Hours turned into a day, then a day and a half. After 36 hours, his worried family found him collapsed in the back garden. His owner recognised the signs immediately – Sox was blocked again.
He was rushed back to the vet, once again in a life-threatening state. The veterinary team stabilised him by decompressing his bladder and placing another catheter. Investigations were repeated – no stones, no infections, nothing obvious to explain the repeated obstructions. But this time something new was clear: Sox’s urethra was very narrow.
By now, Sox and his family were exhausted. These episodes were not only traumatic but also emotionally draining and financially costly. The vet team sat down with his owners to discuss the options.
The first option was to manage the obstruction again and hope for the best. The second was more drastic: a perineal urethrostomy (PU). This surgery involves amputating the penis and creating a shorter, wider urethra, reducing the chance of future blockages. It’s not a decision any cat owner takes lightly. PU surgery doesn’t cure all forms of urinary tract disease, and it can carry risks. But given Sox’s history and the clear narrowing of his urethra, it offered him the best chance of a normal life.
After much thought, everyone agreed surgery was the right path. Sox underwent the procedure, and it was a success. Within a few days he was back home, healing well and gradually resuming his routines. Follow-up checks confirmed the wounds were healing nicely, and Sox was on the mend.
Since then, he hasn’t looked back. His owners continue to keep his stress levels low, sticking with the behavioural changes they put in place years earlier. The combination of surgery and a supportive environment has given Sox a new lease of life – and given his owners peace of mind.
Sox’s story is a reminder of just how complex urinary problems in cats can be. What looks like a simple case of cystitis can, in fact, be a multifaceted condition tied to stress, anatomy, and environment. It also highlights the importance of quick action: both times Sox was blocked, his owner’s speed in getting him to the vet was what saved his life.
Today, Sox is back to ruling his household, enjoying his comforts, and keeping his humans on their toes. Thanks to their unwavering commitment and the dedication of his owner, this six-year-old has many more happy years ahead.
If you would like more information and tips on how to help prevent cystitis in cats, visit our Feline Care Guide page on our website by clicking HERE.

Cosmo’s Courage: A Remarkable Journey Through Tetanus and Recovery
Each of our patients is incredibly special to us, and we care for them as if they were our own. Every so often, however, a patient comes along whose strength of character leaves a lasting imprint on our hearts. One such patient is Cosmo, a Cocker Spaniel who was hospitalised with us for 19 days last November.
Cosmo was brought in on 1st November after his owners noticed he had an unusual facial expression. His expression included a wrinkled forehead with pulled back ears, a stiff jaw (‘lockjaw’) with pulled back lips, and small pupils with both eyes looking outwards. This expression is known as risus sardonicus and is a very characteristic and classic early sign of tetanus. Tetanus is very uncommon in dogs, as they are naturally quite resistant to the disease (cats even more so), but we do occasionally see cases. The condition is caused by bacteria found in dirt or soil entering the body through a wound, leading to severe muscle rigidity and stiffness.
Following admission and during the first week of hospitalisation, Cosmo was treated with antibiotics, muscle relaxants, pain relief (as constant muscle rigidity/spasm is painful) and intensive supportive care. The use of anti-toxin in cases of tetanus is controversial and often considered more risky than beneficial due to the high chance of anaphylactic allergic reactions. Despite his early treatment the condition progressed and the rest of his body and muscles became increasingly rigid. His walk became ever more stilted due to the inability to bend his legs and such dogs suffering from tetanus are described as having a ‘sawhorse stance’. His tail became stiff and pointed and he began having difficulty urinating and eating. A urinary catheter had to be placed to help regularly empty his bladder, along with a feeding tube that allowed us to bypass his mouth due to difficulties with eating and swallowing. His gastrointestinal system was also affected, meaning his stomach and intestines were not moving food through properly. He would intermittently regurgitate the food he was given via the feeding tube and so additional medications were introduced to try and reduce this happening.
The most worrying moment came eight days into his stay, on a Sunday morning, when Cosmo experienced a sudden attack of breathing difficulty. This may have been due to a regurgitation episode affecting his airway, but so severe was his difficulty that the two vets scheduled to be in on that day immediately placed him under anaesthetic. Chest X-rays were taken and thankfully his lungs and airways were clear and over the following 24–48 hours he slowly recovered. From that point on, Cosmo finally began to make gradual but steady improvements each day.
He continued the antibiotics, muscle relaxants, GI medications and pain relief, and his ability to walk finally began improving. Next, he was able to urinate independently, so no further urinary catheterisation was needed. Finally, and most rewarding of all, Cosmo regained the ability to eat by himself, eventually leading to the removal of the feeding tube. He was discharged 19 days after admission, still with some stiffness, but very much on the road to a full recovery. When he was home he developed an unusual but well known sequela to tetanus known as ‘REM Sleep Behaviour Disorder’. This involves ‘nightmare-like’ episodes which occur during light sleep where dogs can twitch, vocalise and paddle, stopping when they enter a deeper sleep. It is experienced by around half of dogs that survive tetanus and whilst it can be alarming, it is not harmful and generally subsides over the following 6 months.
Cosmo’s journey to recovery has been a long and challenging one. It was made possible not only by his incredible determination and the unwavering love and understanding of his owners – whose regular visits were always rewarded with a wagging tail – but also by the outstanding dedication of the entire team at Shepton and Wells Vets. Our vets, nurses, and support staff demonstrated exceptional passion and commitment throughout his care, with special recognition to our nursing team, who provided compassionate, round-the-clock care during his hospital stay, including the night nursing team that we are very fortunate to have here at Shepton Vets to offer care for inpatients 24/7, 365 days a year.
Cosmo’s story is a powerful reminder of what can be achieved through teamwork, perseverance, and a shared commitment to giving every patient the best possible chance.




Uncovering the Cause: Novak’s Unexpected Abdominal Infection
At 10 years old, Novak had always been a healthy cat, so when he suddenly became lethargic and stopped eating, alongside vomiting and diarrhoea, his concerned owner knew something wasn’t right. He was brought to our Wells practice, where our team quickly recognised that Novak needed further investigation and hospitalisation. He was promptly transferred to our Shepton hospital for more in-depth care.
Initial blood tests gave us some clues, but no clear answers as to what was making Novak so unwell. He remained flat and anorexic, so we performed abdominal imaging, which revealed that his intestines were significantly distended with gas. This made us concerned about a possible blockage in his digestive system, although nothing definitive showed on the scan.
With Novak’s condition not improving and the possibility of a blockage still on the table, we discussed our findings with his owner. The only way to know for sure — and to potentially treat the issue — was to perform an exploratory laparotomy, a surgical procedure to open the abdomen and take a direct look inside. Novak’s owner gave their consent for us to proceed and give him a chance.
During surgery, we discovered that Novak’s intestines were inflamed and filled with gas, but thankfully, there was no physical blockage. Instead, we found multiple abnormal pockets — what looked like abscesses — scattered throughout his omentum, a fatty, protective layer within the abdomen that helps isolate infections and supports the intestines and other abdominal organs.
There was also infected fluid present, which indicated that Novak was suffering from peritonitis, a serious and potentially life-threatening inflammation of the abdominal lining, usually caused by infection. In Novak’s case, the inflamed intestines were no longer functioning properly, unable to move food or gas effectively, which explained his symptoms.
We carefully examined his intestines for any perforations, which could have allowed bacteria to escape and cause this infection, but none were found. The abscesses were surgically removed, and Novak’s abdomen was thoroughly flushed with sterile fluid to reduce any remaining bacterial contamination.
To support his recovery, we placed an oesophageal feeding tube, which allowed us to provide nutrition directly until he felt strong enough to eat on his own. Over the next week, Novak began to steadily improve. With time, medication, and gentle care from our team, his appetite returned, and we were able to get him home to his family. After a few more days we were confident enough in his appetite to remove his feeding tube.
Lab results later confirmed that the abnormal tissue was indeed omental abscesses, likely caused by a foreign object, such as a sharp item he may have swallowed or a wound sustained during a fight or accident. Another possibility is that it resulted from a healed intestinal ulcer that briefly allowed bacteria to escape into the abdomen.
Today, Novak is back home and continuing to do well. He’s eating, purring, and enjoying his well-earned rest after such a dramatic illness — and we’re thrilled to see him back to his old self.
This case reminds us how subtle signs in our pets can signal something serious, and how advanced diagnostics, timely surgery, and dedicated post-operative care can lead to a happy ending — even in complex cases.

Adder Bites: Lady’s Encounter
With the sun shining, warmer weather is a great excuse to get out and about with our dogs. However, one thing to be aware of is the risk of adder bites, which although rare, they can be serious.
The European adder, Vipera berus berus, is the only venomous snake in the UK. It’s a protected species and can vary in colour from pale grey to dark brown to reddish brown. The head has a distinct ‘V’ or ‘X’ shaped mark on the top. The adder has a characteristic vertically slit pupil that is helpful in distinguishing it from other British snakes and lizards. Adders generally only bite when provoked or startled. Adder bites usually occur from February to October as they come out of hibernation as the breeding season starts, with the peak time for bites between June and August. They are found in habitats such as heathland, sand dunes, moorland and woodland edges. They are hard to spot, so it can be hard to prevent a bite from occurring. If you are concerned, the safest option is to keep your dog on the lead.
We recently had a visit from Lady, an inquisitive 7 year-old cocker spaniel, who was bitten on the nose by an adder whilst out on a walk in Stockhill woods, near Priddy. Thankfully, lady’s owner saw the snake bite her and acted quickly and calmly, getting her to the car and bring her in to us immediately.
If an adder bite occurs, it is important to try and stay calm and bring transport to your dog, if this is not possible, carry them to the car to keep their heartrate down. This can help reduce the speed in which the venom spreads. DO NOT try to use a tourniquet or ligature (tie) as this can damage the tissue and lead to complications.
On arrival Lady was presenting clinical signs of anaphylactic shock, she had localised swelling to her nose, face and mouth, which continued to spread to her tongue and throat.
An adder bite that has injected enough venom causes significant levels of morbidity (symptoms) but has a relatively low risk of mortality (death). However, as it is unpredictable, a vet check and treatment are always needed. Bites are very painful and can cause significant swelling. Clinical signs can also include lethargy, collapse, vomiting, panting, lameness, bruising and bleeding. Dogs can also show signs of shock such as a high heart rate and blood pressure changes. Bites to the tongue or neck can be life threatening if significant swelling develops. The wounds themselves can have damaged skin which can slough off.
Shepton Vets is a Tox Box registered practice, meaning we keep anti-venom (and other anti-toxin drugs) on site. Antibiotics may also be required. If the skin becomes damaged and starts to die after a few days, this may require surgery to remove it.
Lady was treated with an anti-venom and anti-inflammatories as well as pain relief and intravenous fluids. She responded well to treatment and was monitored here by our out of hours team, overnight. Lady was able to go home the next day with supportive treatments, monitoring for signs of progressive swelling, dyspnoea, anorexia, skin damage, sloughing and necrosis.
Anti-venom is a human based medicine and has to be imported into the UK. In animals at risk of swelling that can compromise breathing it can rapidly reduce swelling by binding to the venom and dramatically reduces hospitalisation time. If you are concerned your dog has been bitten, do not hesitate to contact us.

Crackles, Collapses, and Clues: A Pekingese’s Pulmonary Puzzle
Boodu, a very fluffy 6 kg Pekingese, has been a regular at our practice for over 13 years. He is well known to all the staff for his extreme reluctance to have his nails clipped. However, his recent visit was under very different circumstances.
As with many older animals, Boodu’s mobility isn’t what it used to be. Combined with the heatwaves we’ve had this summer, a bit of slowing down and reduced exercise was to be expected. More recently though, he appeared to be struggling with getting around — particularly when going upstairs — and had collapsed three times within a 24-hour period. He would often pant before collapsing, then lie on his side for a few minutes before getting up and continuing as normal. He didn’t lose consciousness during these episodes, but they became more frequent over a couple of days.
He was initially seen on a Sunday, when a heart murmur and occasional missed beats were detected, raising suspicion of heart disease. As his breathing was still normal when resting, he was scheduled for further investigations the following Wednesday. However, he re-presented on both the Monday and Tuesday as his episodes worsened. By Tuesday, there was noticeable effort to his breathing, the heart murmur remained, and ‘crackles’ were audible when listening to his lungs. These findings were strongly suggestive of left-sided heart failure causing fluid build-up in the lungs, so he was given furosemide — a diuretic — to remove the presumed fluid.
Over the course of the day, however, there was no improvement. In fact, his breathing worsened, which should not have occurred if left-sided heart failure had been the cause.
We opted to perform chest x-rays, which showed no significant fluid build-up or masses. The next step was a heart scan (echocardiogram) to fully assess how the heart was functioning — and the findings were unexpected.
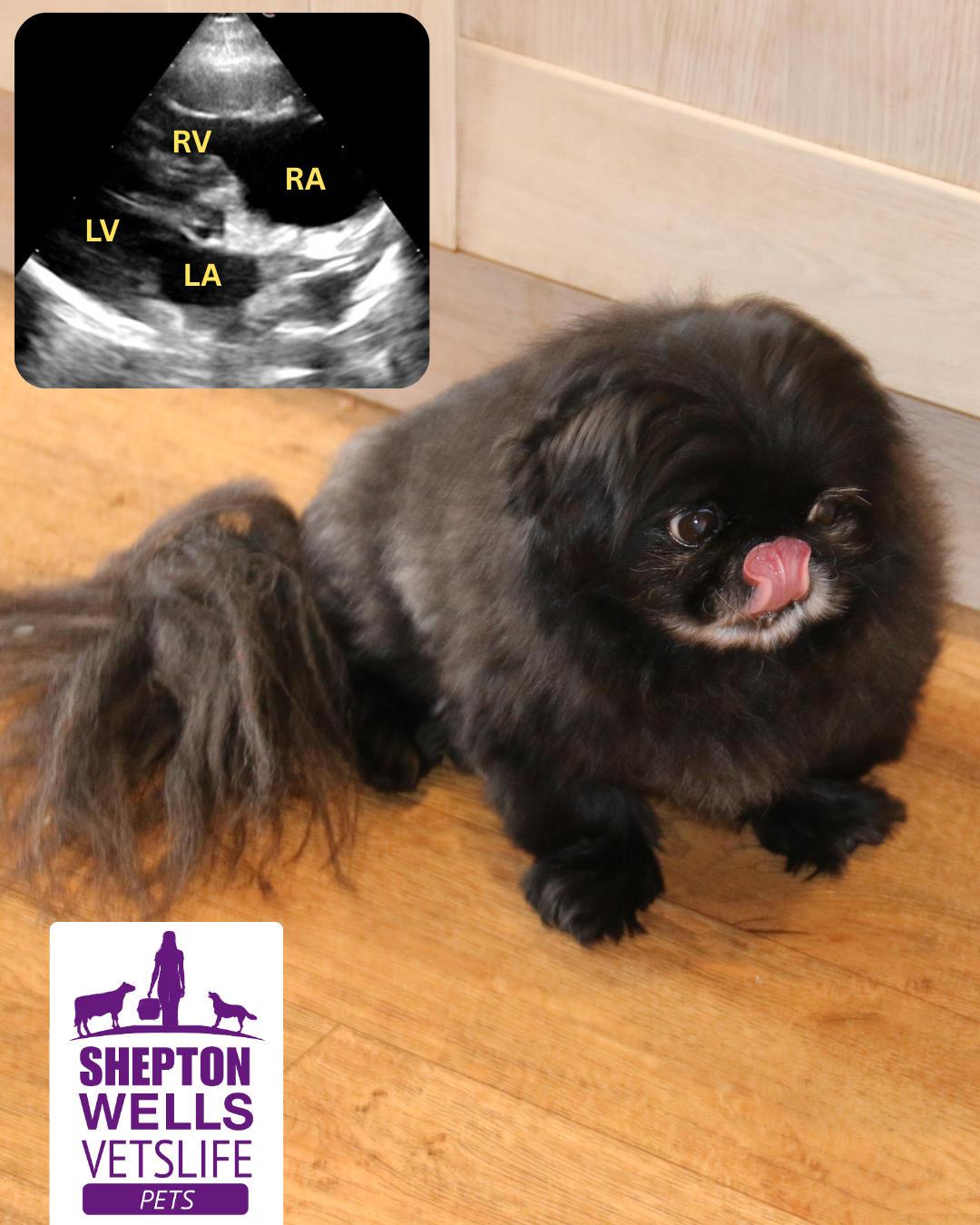
Most heart disease, especially in older small dogs (<20 kg), affects the left side of the heart, often leading to fluid in the lungs and breathing difficulties, as was initially suspected. However, Boodu’s heart showed right-sided changes, with the right-sided chambers larger than the left — a finding that should never occur. Using colour-flow Doppler imaging (see image below), we could see that the one-way valve on the right side of the heart (the tricuspid valve) was allowing blood to flow back in the wrong direction. This can occur due to valve degeneration, increased pressure in the lung’s blood vessels, or sometimes as an insignificant finding in older dogs.
The speed of this backward blood flow was measured using continuous wave spectral Doppler. The pressure was found to be elevated, leading to a diagnosis of pulmonary hypertension — high blood pressure within the lung vessels. Due to this increased pressure, blood from the right side of the heart was struggling to reach the lungs and return to the left side. A lack of blood reaching the left side of the heart means a lack of blood being pumped to the rest of the body, which explains Boodu’s weakness and episodes of collapse.
The next question was: Why had Boodu developed pulmonary hypertension? There are many possible causes, including underlying lung diseases such as bronchitis, tumours, lungworm, or blood clots. The crackles heard earlier in the day were now thought not to be fluid-related, and since no tumours were visible on the chest x-rays, the crackles were likely due to underlying lung inflammation — such as undiagnosed bronchitis. This type of airway inflammation can affect the lung’s blood vessels and lead to pulmonary hypertension.
Treatment and Outcome
Boodu was started on two medications:
- Sildenafil – This is the active ingredient in Viagra. It dilates the lung blood vessels, allowing easier movement of blood from the right side of the heart through the lungs and back to the left side.
- Terbutaline – A bronchodilator that opens the airways, reducing resistance and increasing airflow to the lungs. This was prescribed due to the suspected bronchitis.
He responded very well to treatment. Within a few hours, the crackles previously heard had disappeared and his breathing had returned to normal. He was monitored overnight by our night nurses and discharged the next day, continuing both medications.
We’re pleased to report that Boodu has had no further collapsing episodes since.
A Lump, a Scare, and a Brave Boy Named Bruno
We are all familiar with the advice that we should regularly check ourselves for lumps and bumps. Well for our pets it is no different – although we must do this for them of course! Finding a lump that hasn’t previously been noticed can be a scary ordeal and so, for the owners of Bruno, as soon as they felt an odd lump in his neck back in 2024, they wanted to get him checked out. At the first opportunity they were on the phone to the practice to book him in.
Most of the time we can reassure owners that such new lumps are not a problem, or that we can manage them with straightforward surgery. But the location of Bruno’s lump caused us some concern, so we suggested we sample the lump with a needle, in the hope that the laboratory could analyse the cells and give us some more information.
The results showed that Bruno had a tumour in his thyroid gland, the gland that produces thyroid hormone. These tumours can have the potential to spread and so, after discussion, we decided we should see Bruno to stage his condition – to effectively establish if there were any signs of tumour spread elsewhere in his body.
Bruno, oblivious to all that was going on and as lively and friendly as ever, visited the practice again in the next few days and was sedated so we could perform x-rays of his chest, a scan of his abdomen, and sample his lymph nodes. There was good and bad news. The good news was that there was no sign of spread of the tumour to his internal organs or lymph nodes. The unwelcome news was that we identified that both his thyroid glands were affected by the tumour.
Having no other signs of tumour spread is always fantastic news. Having tumours in both thyroid glands though was a problem – if we wanted to operate then it made surgery very complicated. The reason for this is that the thyroid glands sit very close to another gland, the parathyroid gland, which control blood calcium levels. Performing surgery to a thyroid gland runs the risk of injuring the adjacent parathyroid gland, which is manageable if the surgery is done on just one side, as the opposite gland will still function and control calcium levels. But if both parathyroid glands are damaged the patient can be left unable to control blood calcium levels, which can be life-threatening.
We had to plan carefully for how we proceeded with treatment for Bruno, and part of this was discussing Bruno’s condition with an external specialist oncologist who frequently advises us on complicated cancer patients. After a review of all of Bruno’s information we felt that surgery, to try and carefully remove both of Bruno’s thyroid glands, was the best approach. However, the risks of the surgery were significant and so we needed to discuss the potential complications in detail with Bruno’s owners.
Bruno’s owners were understandably concerned but knew that any treatment carried certain risks, and if left alone the tumours would spread in the end. Ultimately, they had no doubt that they wanted to try to treat Bruno’s cancer and so, whilst nervous, they wanted him to have the surgery.
With the potential risk of causing low blood calcium levels this wasn’t a surgery to schedule for any given day. It needed to be well planned and we needed to be prepared, both with time and all the necessary medication, for the complications that may occur.
Bruno was admitted at the start of a week and his procedure was scheduled for first thing. We had prepared the day and night teams for the monitoring he would require and had a plan for his anaesthesia and recovery. His surgery commenced mid-morning and we had the task of excising both cancerous thyroid glands whilst attempting to identify, and protect, his tiny parathyroid glands.
The surgery took a while but could not have gone better. With time, a lot of care, and the use of a vessel sealing devise to stop any small bleeds, we felt we had managed to retain the essential parathyroids. Bruno had local anaesthetic applied to his wounds as they were closed and before long, he was waking up in bed.
His owners were given the good news, but equally advised he wasn’t out of the woods. We needed to monitor his blood calcium levels over the next couple of days, and if all was well then, he could go home.
Bruno did brilliantly, with his blood tests all showing normal parameters and him being bright in demeanour. As such he went home, and we awaited the results of the definitive biopsies from his thyroid glands. This was a process of confirming the diagnosis but would also give an insight into how aggressive the tumour may be.
The results returned to confirm a thyroid carcinoma as suspected, but also that it showed features indicating that it was of a grade that was very likely already starting to spread. However, this was no surprise, we already knew it was likely and, with the help of the oncologist we had a plan for the next stage of Bruno’s treatment. This was to offer a course of chemotherapy to him as monthly injections, aiming to try and kill any potentially spreading tumour cells in his system.
For our animal patients we accept that chemotherapy can be daunting. However, our aim is to administer treatment in a way that doesn’t affect quality of life, but still extends it. Being unwell for long periods isn’t acceptable with pets and when this was all discussed Bruno’s owners were once again happy to proceed with treatment.
Bruno finished his 6 months of chemotherapy and was doing well – receiving a replacement thyroid hormone and otherwise living a very normal life – which for him involves a good number of coastal walks and a lot of love from his owners.
Unfortunately, in April 2025, Bruno’s lump in his neck recurred. In May, this was biopsied, and was again confirmed to be cancerous. However, we are pleased to report that this was successfully removed in entirety in June and he has since recovered very well and now has thyroid supplementation with periodic monitoring. So far there are no signs of another relapse and hopefully Bruno has fought these lumps for good!

Tiggy the Irish Terrier – An unusual case
This week’s case is a one off for me, and the diagnosis was, unusually, aided by my husband’s garden wall-building activities (more of that later).
The lovely Irish Terrier, Tiggy originally came in and saw vet Carmen as she had been vomiting and had some diarrhoea with a little bit of fresh blood. This is quite a common case that we see day to day. After examining her, Carmen prescribed the appropriate medication for her signs.
Four days later she came back in on a Sunday afternoon and saw vet Sarah as she had become more poorly. Although still quite bright and keen to eat she had vomited a considerable amount of pure blood and was passing tarry black diarrhoea as well. This is a sign of bleeding in the stomach or upper small intestine as the blood is then semi-digested and comes out with a characteristic black appearance.
I was worried about the amount of blood that she may have lost as her gums and tongue were quite pale rather than a nice healthy pink colour. We talked about any possible toxins that she may have eaten, and the owner couldn’t think of any, but did remark that they had recently moved into an old cottage and were having quite a lot of renovations done. They had lime plaster on the walls and Tiggy was licking at this and the lime dust that was coming off the walls.
Here’s where the gardening comes in. I had recently become aware of just how caustic lime products can be as my husband is using lime mortar to build a wall in our garden and only the day before had shown me how it had burned through the skin on his hand where there was a small hole in his glove. I was suspicious that this could be the cause of the irritation and bleeding in Tiggy’s gut.
We admitted her and started her on intravenous fluids and several medications to try and help her gut to heal. The next day was an anxious time as Josh performed an ultrasound on her to make sure that there was no sign of a tumour that could also have been responsible for the bleeding, particularly as Tiggy is 11 years old. Fortunately, nothing abnormal was seen.
We had been monitoring Tiggy’s red cell count closely as that gave a good idea as to whether she was continuing to bleed, and that continued over the next few days with Tiggy coming in for daily visits. For a couple of worrying days, it hovered just above the level where we would need to consider a blood transfusion, but then she gradually began to turn a corner. Her appetite improved, she stopped vomiting and was passing normal poos.
We finally signed her off nearly 2 weeks after her 1st visit as she was back to normal and had a very healthy red cell count. The only problem now is making sure she stays away from the renovations!












